MELASMA & HYPER-PIGMENTATION Treatment in Chelsea & Battersea
Skin pigmentation concerns like melasma and hyperpigmentation can significantly impact your confidence.
At Derm Design we off the best melasma and hyperpigmentation treatment in Chelsea & Battersea. We specialise in offering tailored solutions to restore your skin’s natural glow and even tone. Our experts use the latest treatments and advanced technology, ensuring effective, safe, and personalised care.
types of HYPER-PIGMENTATION & Their Causes
Hyperpigmentation refers to darkened patches or spots on the skin caused by excess melanin production. This condition has various forms, each with unique triggers and characteristics. Understanding these types is essential for accurate diagnosis and effective treatment
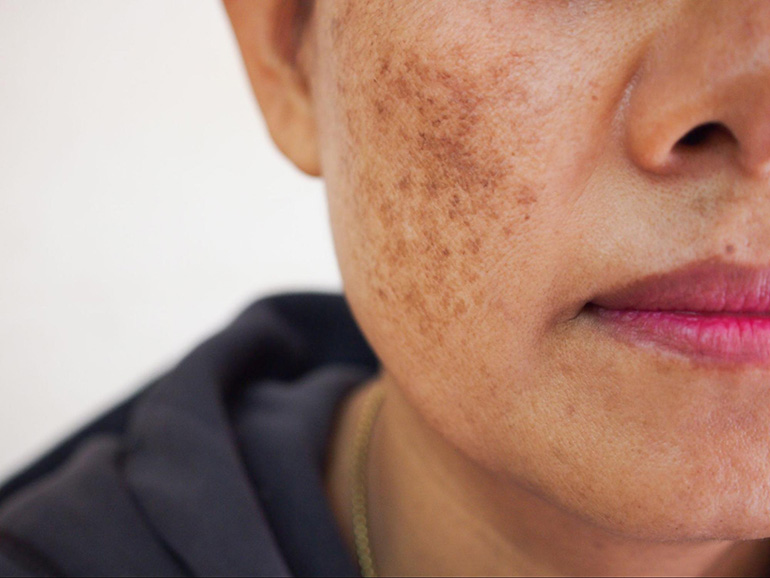
Melasma: Hormonal and Sun-Triggered Hyperpigmentation
Melasma is a common type of hyperpigmentation, often appearing as dark, patchy areas on the face, neck, and forearms. This condition is predominantly seen in women and is frequently associated with hormonal fluctuations such as:
- Pregnancy (also known as the “mask of pregnancy”).
- Use of birth control pills.
- Hormonal shifts during menopause.
Additionally, UV exposure significantly exacerbates melasma, making sun protection a critical component of management.
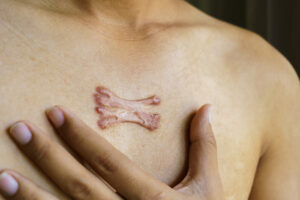
Post-Inflammatory Hyperpigmentation (PIH)
PIH occurs when the skin darkens after inflammation or injury. Common triggers include:
- Acne: Dark spots or uneven patches may appear after active breakouts heal.
- Eczema or Psoriasis: Flare-ups can leave behind residual pigmentation.
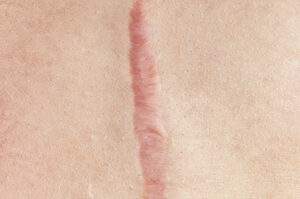
- Skin Trauma: Wounds or scratches can result in localised dark spots.
Unlike melasma, PIH often presents with uneventextures alongside pigmentation.
Freckles: A Genetic Type of Hyperpigmentation
Freckles, or ephelides, are small, flat, brown spots often seen on areas exposed to the sun. They tend to be inherited and become more prominent after sun exposure. While harmless, they are a frequent cosmetic concern for individuals seeking a more even skin tone.
Sunspots: Age and Sun Exposure Combined
Also referred to as age spots or solar lentigines, sunspots are flat, brown marks that develop after years of cumulative sun exposure. They commonly appear on areas most exposed to sunlight, such as:
- Face
- Hands
- Shoulders
These spots are typically associated with aging but are also preventable with proper sun protection.
Hyperpigmentation Caused by Medications
Certain medications can lead to hyperpigmentation as a side effect. Examples include:
- Antibiotics such as tetracyclines.
- Chemotherapy agents used in cancer treatment.
- Anti-seizure medications like phenytoin.
Identifying medication-related pigmentation is crucial, as discontinuation or adjustment may be required to manage the condition effectively.
Signs and Symptoms
- MELASMA: Typically appears as symmetrical brown or gray-brown patches on the cheeks, forehead, nose, and upper lip.
- HYPERPIGMENTATION: Manifests as dark spots or patches resulting from acne scars, sun exposure, or inflammation.
Early intervention is key to effective treatment. If you notice changes in your skin pigmentation, consulting a specialist can make a significant difference.
Related TREATMENTS
Why Choose US
Frequesntly Asked QUESTIONS
There are several factors that can trigger hyperpigmentation, including:
- Sun Exposure: Exposure to ultraviolet (UV) radiation from the sun stimulates melanocytes to produce more melanin in order to protect the skin from damage.
- Hormonal Changes: Hormonal changes during pregnancy, menopause, and taking birth control pills can trigger the overproduction of melanin, leading to a condition called melasma.
- Inflammation: Skin inflammation caused by conditions such as acne, eczema, and psoriasis can trigger melanocytes to produce more melanin.
- Injury: Injuries to the skin, such as cuts, burns, and insect bites, can also cause hyperpigmentation as part of the healing process.
- Genetic Factors: Some people may be more prone to hyperpigmentation due to genetic factors.
Overall, hyperpigmentation occurs when there is an imbalance in melanin production, leading to an accumulation of melanin in certain areas of the skin.
The exact cause of melasma is not well understood. However, there are some risk factors involved in developing melasma, including:
- Hormonal changes: Melasma is often triggered by hormonal changes, such as while taking birth control pills, during pregnancy, menopause, or being on hormone replacement therapy.
- Sun exposure: Exposure to ultraviolet (UV) radiation from the sun can trigger melasma or make it worse. This is because UV radiation stimulates the production of melanin in the skin, which can lead to the development of dark patches.
- Genetics: Genetics play roles in developing melasma in some people predisposed to developing melasma than others.
- Ethnicity: Melasma is more common in people with darker skin tones, such as Hispanic, Asian, or African descent.
- Cosmetics and skincare products: Certain cosmetics and skincare products can irritate the skin and trigger melasma in some people.
While melasma is not a serious medical condition, it can be a cosmetic concern for some people. The best prevention is to avoid known triggers, such as sun exposure, and to use sunscreen daily. If you are pregnant or taking hormonal medications, talk to your healthcare provider about ways to reduce your risk of developing melasma.
The most common treatment for melasma involves a combination of topical medications, sunscreen, and lifestyle changes.
Here are some of the treatments used for melasma:
- Topical medications: Hydroquinone is the most commonly used medication for melasma treatment. It is a skin-lightening agent that inhibits melanin production. Other commonly used medications include tretinoin, azelaic acid, and kojic acid.
- Sun protection: Sunscreen is a crucial part of melasma treatment, as exposure to the sun can worsen the condition. Patients are advised to use broad-spectrum sunscreen with an SPF of 50 or over and to wear protective clothing such as hats and sunglasses.
- Chemical peels involve applying chemicals which exfoliate the outer layers and remove the dark spots. This treatment is usually done by a dermatologist and can help improve melasma's appearance.
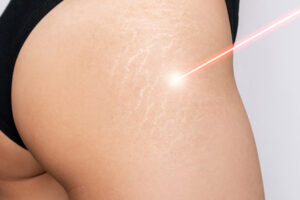
- Laser therapy: using a high-energy laser to remove the dark spots. This treatment can be effective for some patients, but it is not suitable for everyone.
- Lifestyle changes: Certain lifestyle changes can help to improve melasma, such as avoiding exposure to the sun and wearing protective clothing, avoiding hormonal medications or contraceptives, quitting smoking, and managing stress.
It is important to note that melasma can be a complex condition to treat, and it may take several months of consistent treatment before significant improvement is seen.
Results vary based on the treatment type and skin condition. Visible improvement is typically noticed within a few weeks, with optimal results achieved after multiple sessions.
While some topical products can help, professional treatments are more effective for persistent or severe pigmentation issues.
OUR
CLIENTS SAY
CALL BACK
Request
Opening
HOURS
Monday – Friday 9.30 to 17.30
Saturday 9.30 to 18.30
Sunday CLOSED
CONTACT
Details
-
Ground Floor, Riverfront
368 Queenstown Rd London
SW11 8NN -
Tel: 0207 941 8320
-
info@derm-design.com
Trending BLOG POSTS