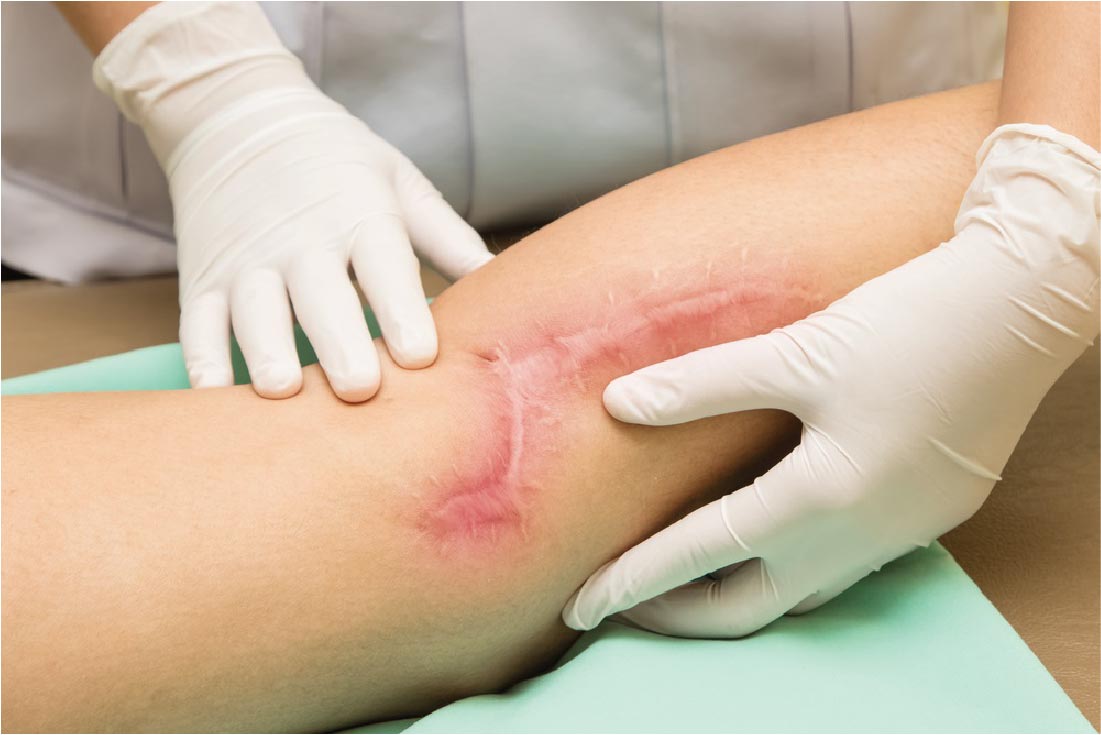
Scar Treatment
Welcome to our premier scar treatment services in London, where we recognise that scarring is an inevitable outcome following skin wounds or injuries. When your skin undergoes trauma, the body initiates a natural healing process, producing collagen fibers to close and mend the affected area, ultimately leading to the formation of visible scars.
Notably, scarring becomes more pronounced when the injury extends to the dermal layer of the skin, triggering collagen production as a crucial part of the body’s intricate healing mechanism. While essential for restoration, this process often leaves behind noticeable scars.
Inflammatory responses to skin damage may manifest as redness, dark spots, and patches of grey or brown. In severe cases, persistent inflammation poses a risk of permanent scarring on the healed skin surface.
The severity and appearance of scars are contingent upon the intensity of the initial skin injury, the location on the body, and the age at which the injury occurs. While complete eradication of scars is not feasible, our comprehensive scar treatment in London provides effective methods to minimise their size and enhance their appearance for long-term relief.
Scars present diverse complexities, necessitating specialized treatments tailored to the specific scar type. Your age and the scar’s duration are critical factors influencing the most suitable treatment plan. Precise scar diagnosis is paramount before initiating any medical procedure to ensure optimal results without exacerbating the condition.
Choose our scar treatment services in London for a personalised and effective approach to scar management, led by experts in the field. We are dedicated to providing solutions that address your unique needs, optimising results, and delivering lasting relief.
Frequently Asked Questions
What Are the Types of Scars?
There are several different types of scars, including:
Colour changed: After skin inflammation subsides, post-inflammatory colour change of the area may be observed. Although they will improve over time, it could take several months to vanish completely.
- Red, pink or purple marks: Post-inflammatory erythema (PIE) is the aftermath of inflammation, leaving behind distinct red, pink or purple spots. Blood vessel dilation and damage due to the inflammatory process can lead to these discolorations on your skin that may take up to 6 months to vanish entirely.
- Brown, grey, or dark marks: Post-inflammatory hyperpigmentation (PIH) is a temporary pigmentary alteration caused by skin trauma or inflammation. Melanin overproduction leads to darkening of specific areas on the face and body. It is typically seen more often in those with darker complexions. PIH can occur alongside post-inflammatory erythema (PIE) yet may last longer than PIE does for some individuals.
- White marks: Post-inflammatory hypopigmentation is a characteristic loss of natural skin pigment after an injury to the area has healed. It results from destruction or damage incurred during the healing process on melanocyte cells, which are responsible for producing pigments in our skin. This condition is especially noticeable and more obvious in people with darker complexions but can occur on any skin phototype.
Texture changed:
- Normal fine-line scars: Minor wounds such as cuts will often heal to form a raised line that gradually flattens and fades out over two years. Unfortunately, the scar will not completely disappear, leaving a visible mark or line. Fine-line scars are common after a wound or surgery. Though typically not painful, some might feel itchy for months afterwards.
- Pitted or sunken scars: otherwise known as Atrophic scars, are caused by the skin’s inability to regenerate new tissue. These types of scars generally form after certain skin conditions like acne and chickenpox but can also be developed due to an injury that leads to fat loss under the skin. These scars often leave an emotional scar in addition to a physical one.
- Raised, thick and lumpy scars: Keloid scars and hypertrophic scars are both types of raised scars that form due to an overproduction of collagen during the healing process. However, they differ in their appearance, size, and location.
What Are the Difference Between Keloid and Hypertrophic Scars?
Keloid and hypertrophic scars are both raised scars that form due to an overproduction of collagen during the healing process. While they share some similarities, there are important differences between the two:
Keloid scars:
- Appearance: Keloid scars are thick, raised scars extending beyond the original wound’s boundaries. They are often shiny and have smooth surfaces.
- Size: Keloid scars can be quite large and can continue to grow over time. They may also be challenging to treat due to their size.
- Location: Keloid scars can occur anywhere on the body, but they are more common in areas where the skin is under tension, such as the chest, shoulders, earlobes, and along the jawlines. If you are predisposed to keloid scarring, it may appear in multiple locations.
- Risk factors: Keloid scars are more common in people with darker skin tones and tend to run in families.
Hypertrophic scars:
- Appearance: Hypertrophic scars are also thick, raised scars, but they do not extend beyond the boundaries of the original wound. They have a more flattened appearance compared to keloid scars.
- Size: Hypertrophic scars tend to be smaller than keloid scars, and they typically do not continue to grow over time.
- Location: Hypertrophic scars can occur anywhere on the body, but they are more common in areas where the skin is under tension, such as the chest, shoulders, and earlobes.
- Risk factors: Hypertrophic scars can occur in people of any skin tone and tend to occur more frequently in younger people.
Treatment options for both keloid and hypertrophic scars may include corticosteroid injections, laser therapy, silicone dressings, and surgery. It is important to work with a dermatologist to determine the best treatment plan for your specific case of raised scarring.
How Can a Keloid be Treated?
Unfortunately, Keloids are still incurable. Nevertheless, there are ways to help flatten them and reduce the associated discomfort. No one treatment method has been proven better; in fact, keloids often tend to recur after treatment. While there is no one-size-fits-all treatment for keloids, several options may be effective in reducing their size and appearance.
- Steroid Injections: Injections of corticosteroids, such as triamcinolone into the keloid can help flatten and shrink keloids. The injections are typically given every few weeks, and multiple treatments may be necessary. Side effects, steroids can make the skin thin, fragile and pale.
- Applying a strong steroid cream or steroid-containing tape.
- Silicone sheets or gels: can be placed over keloids to reduce their size and appearance. They work by hydrating the skin and creating a barrier that helps to reduce collagen production. This method is safe and can be effective if used for several months.
- Compression with bandages or devices (such as clips or splints) may sometimes help, particularly on the earlobe and for keloids on the torso.
- Surgery: Surgical removal of keloids is an option, but there is a risk that the keloid may recur or become even more extensive. To reduce the risk of recurrence, surgeons may use corticosteroid injections or radiation therapy in conjunction with the surgery.
- Radiotherapy can be used after the surgical removal of keloids to reduce the risk of recurrence. It can also be used as a standalone treatment to shrink keloids. However, it has a small risk of causing skin cancer due to radiation exposure. Therefore, this treatment is rarely prescribed.
- Cryotherapy involves freezing the keloid with liquid nitrogen, which can help to reduce its size and flatten it. This method can effectively treat medical conditions, either on its own or in combination with other treatments. However, it is essential to note that cryotherapy may cause a temporary loss of skin pigmentation.
- Laser therapy can be used to reduce the size and redness of keloids. It works by targeting the blood vessels that supply the keloid with nutrients. This method is effective for maximum results, especially when paired with steroid injections.
How Long Does It Take for Steroid Injections to Work?
Steroid injections are commonly used to treat hypertrophic and keloid scars, as they can help to reduce inflammation and flatten the scar.The time it takes for steroid injections to work on scars can vary depending on the individual and the severity of the scar.
After the injection, you’ll feel a softening of the scar, and your discomforting symptoms, like pain and itching, will decrease several days afterwards. In some cases, patients may notice a reduction in the size and redness of the scar within a few days of the first injection. However, it typically takes several weeks to see significant improvement.
Patients may require multiple injections over several weeks or months to achieve the desired result. The frequency of the injections will depend on the severity of the scars and the individual’s response to treatment.
After multiple injections, the scars usually become less visible and flatten within three to six months. In instances with bigger or more resistant lesions, it might take longer for this process to occur. The full effect of the treatment may not be apparent for several months as the scar continues to heal and collagen production slows down.
It is important to work closely with a dermatologist or plastic surgeon who has experience treating scars to determine the best treatment plan for your individual case.
What Are the Side Effects of Steroid Injections?
Though it is possible to experience a few mild side effects, these usually resolve over time. You could experience the following.
- Pain: The introduction of steroids to the scar can cause soreness, with discomfort lasting up to 48 hours. If needed, paracetamol is an effective and safe pain relief option.
- Bleeding: It is not uncommon to witness small bleeding after the injection. To prevent further complications, keep your adhesive plaster on until it ceases.
- Atrophy: The tissue around the scar contracts, causing an indentation in the skin. This phenomenon is known as shrinkage.
- Hyper/hypopigmentation: Steroid injections can sometimes cause changes to the skin’s pigmentation, causing either lightening (hypopigmentation) or darkening (hyperpigmentation)of the skin.
- Telangiectasia: Sometimes, small reddish spots known as purpura can become visible around the injection site. This is due to an enlargement of microscopic blood vessels in that area.
Dr Miller is here to help
Scars can vary widely and require tailored treatments, depending on your age and how long you’ve had the scar. It is essential to determine precisely what type of scar it is before selecting a treatment approach- using an incorrect procedure might aggravate its look.
Dr Miller has extensive experience treating all types of scars using many treatment modalities. At the consultation, she will examine your scars and determine the best course of treatment based on factors such as the type of scars you have, their location, size, and severity, as well as your skin type and medical history.
She will work with you to develop a personalized treatment plan that takes into account your individual needs and goals. She will also provide guidance on aftercare and follow-up appointments to ensure that your treatment is effective and that you are happy with the results.